Sådan fungerer menneskelig eksperimentering

Det er det fjerde århundrede f.Kr. og Herophilus, anatomiens fader, hæver sit kirurgiske blad for at skinne i den egyptiske sol. Rundt omkring ham stimler læger fra hele Middelhavet ind for at se hans snit, og de anstrenger sig for at se, mens han bøjer sit instrument til den opgave, der ligger forude. Allerede nu har de lært så meget om øjets fysiologi, har kastet mysterierne om menneskelige indvolde ned.
Endnu en gang kommer mesterdelene kød ind i den blodige labyrint af arterier og muskler. Med hvert snit vrider kroppen sig nedenunder af smerte, spænder mod snorene, der binder ham til operationsbordet - for han er ikke blot et kadaver, men en levende, åndedrætsprøve. Herophilus fortsætter sin undersøgelse, uvidende om den dømte fanges dæmpede skrig. De lærde diskuterer studiet af de udsatte poroi eller nerver, selvom de gnister af ufattelig pine.
Det var en tid med stor lærdom i den antikke verden, og Alexandria var selve centrum for den. Ptolemæus-familien havde etableret et museum eller "musernes hus" til fremme af videnskab og litteratur. Familiens fund var med til at fylde det legendariske bibliotek i Alexandria, og i en periode fungerede byen som et skræk mod en uvidenhedsskygget verden. Forbuddet mod dissektion af kadavere blev ophævet.
I en periode på cirka 50 år blev selv den tabubelagte praksis med menneskelig vivisektion almindelig praksis. Forskere kunne trods alt kun lære så meget af en undersøgelse af de døde. I en tid, hvor man stadig troede, at blodkar transporterede luft, var de nødt til at åbne levende kroppe for deres videnskabelige undersøgelse. Hvorfor skulle de dømtes forladte liv ikke komme kommende generationer til gode?
Herophilus har angiveligt dissekeret næsten 600 levende fanger og opnået sin plads i medicinsk historie med sine forskellige opdagelser. Alligevel udtrykte mange kritikere selv på det tidspunkt uro over vivisektion, uanset belønningen. Hans skrifter gik tabt for altid i 272 e.Kr., da byens store bibliotek blev ødelagt af brand.
Mens vi stirrer tilbage gennem tiderne, står Herophilus næppe som et fjernt flimmer af moralsk dilemma. Historien slanger sig snarere med utallige og foruroligende eksempler på menneskelige eksperimenter.
Det moderne samfund er kun årtier fjernet fra nogle af de værste eksempler på uetiske eksperimenter. Selv i dag fortsætter lægevidenskaben med at udvikle sig på ryggen af menneskelige forsøgspersoner.
Indhold
- Hvorfor eksperimentere med mennesker?
- The Dark Side of Science:Unit 731 and Nazi-Tyskland
- Visdom ud af lidelse:at lære af menneskelige eksperimenter
- Eksperimentering af ukendte emner
- Moderne kliniske lægemiddelforsøg
- Kontante penge til menneskelige marsvin
Hvorfor eksperimentere med mennesker?

Spørgsmålet om menneskelige eksperimenter kommer generelt ned til en grundlæggende kendsgerning:Når videnskab beskæftiger sig direkte med mennesker, er du nødt til at studere mennesker - til sidst. Så enkelt er det. Uanset om du søger at helbrede lidelser og skader, bygge en mere sikker bil eller designe et mere dødbringende våben, skal du muligvis teste menneskelige tærskler for sygdom, stress og skader.
Et par andre muligheder (og etiske forhindringer) har en tendens til at præsentere sig selv, før du tager Herophilus' ledelse og begynder at skære i dømte forbrydere. Hvis dit eksperiment absolut kræver brugen af et menneskeligt emne, kan du altid falde tilbage på den døde sort. Selv uden funktion har du form. Anatomiens berømte fader brugte dem selv til meget af sin forskning.
For at bryde nye veje måtte medicinske pionerer ofte være afhængige af ligene af henrettede kriminelle eller stjæle lig fra grave og gibbets. Body snatching blev en vækstindustri i det 19. århundrede, da medicinske skoler krævede friske kroppe for unge kirurger at øve sig på. I dag kan forskere og studerende lettere få adgang til lovlige medicinske kadavere.
Nogle gange kræver videnskabsmænd et levende emne - en arbejdsmodel. I mange tilfælde henvender de sig til resten af dyreriget. Alene i det seneste århundrede har chimpanser, kaniner og andre dyr hjulpet med alt fra polioforskning og rumudforskning til kosmetik og biovåbentestning.
Bortset fra moralske og etiske dilemmaer er der to centrale problemer med dyreforskning. For det første kan en kanin kun give adfærdsmæssig og fysiologisk feedback. Selv den smarteste primat kan ikke udfylde en Q&A. For det andet arbejder du med en ikke-menneskelig art, hvilket gør det vanskeligt eller umuligt at studere visse menneskespecifikke sygdomme, lidelser og scenarier.
Selveksperimentering har ofte vist sig at være et meget vellykket (og dumdristig) middel til videnskabelig undersøgelse. Adskillige videnskabsmænd har med vilje inficeret sig selv med sygdom eller parasitter for at få et førstehåndsindtryk af emnet. Pierre og Marie Curie modtog Nobelprisen i fysik i 1903 for deres strålingsforskning, som involverede tapning af farlige radiumsalte til deres hud.
Alligevel har selveksperimentering sine grænser. Herophilus kunne ikke have udført sin egen vivisektion, meget mindre 600 separate procedurer på sig selv. Et eksperiment er trods alt kun en fase i den videnskabelige metode - der er ingen mening i at dø halvvejs. Plus, hvordan bevarer du funktionalitet og objektivitet, hvis du lider af selve den pest, du håber at kurere?
Det efterlader menneskelig eksperimentering og alle de negative konnotationer, der følger med det.
The Dark Side of Science:Unit 731 og Nazityskland

Human experimentation doesn't have to be an exercise in cruelty, yet we're not even a century removed from some of the more deplorable acts -- cases that could easily rival and even surpass the alleged crimes of Herophilus and his colleagues.
As in ancient Alexandria, scientists and doctors have often turned to the disenfranchised when the need for test subjects arises. After all, we experiment on animals by telling ourselves that the greater good outweighs the desires of a few lesser creatures. History has shown us where this line of thinking can lead when we see other humans as the lesser creatures in question.
J. Marion Sims is widely considered the father of gynecology and even became the president of the American Medical Association in 1876. Yet Sims developed his experimental surgeries by testing them on African slaves, often without anesthesia.
The United States often turned to prisoners for medical tests, such as the 1906 cholera experiments in the Philippines and the 1915 pellagra experiments in Mississippi. Poor and orphaned children suffered similar fates. In 1908, three Philadelphia physicians infected several orphans with tuberculosis, permanently blinding several. Between 1919 and 1922, Dr. Leo Stanley injected 656 prisoners at San Quentin Prison with animal testis trying to slow or reverse ageing [source:Lunenfeld]. Before the 1970s, roughly 90 percent of all pharmaceutical products were tested on prisoners [source:Proquest].
Yet when it comes to experiments on captives and prisoners, few examples resonate as strongly as the experiments conducted by the Nazis during World War II on Jews, gypsies and other targeted individuals. The doctors conducted cruel and often lethal experiments into wartime injury treatment generally by inflicting said injury on a captive patient. They froze victims to research hypothermia, placed them in compression chambers to test the effects of high-altitude flight. They also conducted brutal sterilization experiments in the name of racial superiority.
Similarly, Japan's infamous Unit 731 reportedly killed more than 10,000 Chinese, Korean and Russian prisoners of war to research and develop biological weapons. They infected inmates and performed vivisections on them, all in an attempt to craft even deadlier weapons out of disease.
How are we supposed to process such atrocities? And what do we do with the data gleaned from degradation and torture?
Wisdom Out of Suffering:Learning from Human Experimentation

Humanity continues to march on through the years, bound to the linear procession of time. Any sober, honest glance back at the path we've traveled is often as horrifying as it is wondrous. Our collective history bristles with atrocity. We can't separate ourselves from it without also draping ourselves again in the cloak of ignorance.
Much the same can be said of science. While it continues to light the way to the future, portions of its momentum were purchased through horrible deeds. But what can we do? No one is arguing that we throw out everything we know about human anatomy in penance for Herophilus' vivisections.
Allied scientists faced such a dilemma at the end of World War II. What were they to do with Unit 731's medical findings on disease? Regardless of the methods used to obtain it, the information was valuable. It was like pondering a gold coin fetched from a vat of boiling oil. Were the U.S. scientists simply to flip it back into the searing pitch? Rather than see the information fall into the hands of the Russians, the U.S. bargained with the Japanese officers responsible:immunity from war crime prosecution in exchange for the ill-gained data [source:McNaught]. The officers were even given stipends.
Similar concerns have arisen concerning Nazi documents leftover from the Holocaust. With no regard for the welfare of their test subjects, German scientists at Dachau subjected victims to extremely low temperatures -- often resulting in death. Yet the Nazis also used these experiments to determine the best method of reviving hypothermia patients in tubs of hot water. Hypothermia researchers later insisted that the data was valuable, no matter how deplorable the methods used to obtain it.
Many critics argue that by using the data, we validate the crimes. Yet purely logistical criticisms arise as well. Can we trust Nazi doctors who sought politically motivated results, such as those that "proved" German racial superiority? In many cases, the experiments lacked proper methods and protocol. The subjects themselves, selected from the death camps, tended to be imperfect specimens to begin with, already suffering from malnourishment and psychological trauma.
Sometimes, however, the victims of atrocity have managed to obtain useful data from the conditions brought on by their tormenters. Jewish doctors documented starvation in the Warsaw ghetto -- notes that later aided the study of hunger-associated disease [source:NOVA].
Experimenting on Unknowing Subjects

We tend to place a great deal of trust in our physicians. With that trust comes the understanding that they won't secretly experiment on us. But there was a time when entering a teaching hospital as a patient might result in not only the procedure you needed, but also whatever the students needed to practice that week [source:Roach].
While the prospect of receiving an unmerited appendectomy at no extra cost may seem horrifying enough, more shameful experiments litter medical history. In 1932, the U.S. Public Health Service began its 40-year Tuskegee study of syphilis. During this time, African-Americans who sought treatment for the disease were deceived. Instead of administering proper medical attention, the doctors allowed their conditions to worsen in order to better study the illness. The U.S. military also tested unsuspecting patients, exposing citizens to germ warfare agents and LSD in the '50s and '60s. Various U.S. radiological tests also used unknowing subjects, injecting hospital patients with plutonium and feeding radioactive cereal to mentally disabled children [source:Proquest].
Human trials became increasingly essential to the pharmaceutical industry as the U.S. Food and Drug Administration began requiring stricter testing of new drugs in the 1930s. In 1966, the National Institutes of Health (NIH) established the NIH Policy for Protection of Research Subjects. This measure established review boards to monitor human experimentation. To this day, U.S. colleges and universities that perform any kind of human experimentation also have institutional review boards , or IRBs .
Subsequently, the National Commission for the Protection of Human Subjects of Biomedical and Behavioral Research (later the President's Commission for the Study of Ethical Problems in Medicine and Biomedical and Behavioral Research) entered the picture to refine the laws and practices surrounding human experimentation.
Throughout the 20th century, medical laws raced to keep pace with human experimentation -- often falling troublingly behind. For instance, 1964's Helsinki Declaration by the World Medical Association allowed for experimentation on incapacitated and incompetent individuals so long as legal guardians gave written consent.
Yet, even sheathed with the protection of signed written consent, human testing continues to bring up ethical concerns.
Modern Clinical Drug Trials
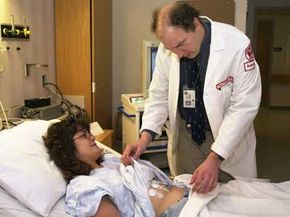
Walk into a Phase I U.S. clinical trial for a new drug and you'll likely find something between a frat house rec room and a hospital. Far from suffering, most of the test subjects would likely be busy watching TV or blasting through a few video games. As it turns out, catheters, needles and the occasional invasive surgical procedure don't really spoil a good time, especially when you're getting paid for it.
These mini-vacations for science can last anywhere from days to weeks and can pay in the thousands of dollars. Sometimes they're even held in hotel rooms. Phase I clinical trials typically involve otherwise healthy (though generally not gainfully employed) individuals. In this stage, researchers try to pinpoint dangerous side effects and potential complications. Phase II trials deal with dosing and efficiency, while Phase III trials enlist the help of actual patients to compare the experimental treatment to conventional ones, placebos or both.
A great deal of money and time go into these tests because pharmaceutical companies have a limited window to get a new drug out on the market and profit from it. U.S. drug patents only last 20 years; if a new medication is tied up in testing for a decade, then it will only have 10 moneymaking years left in it. While the companies themselves are frequently criticized for their commercialism, it does take a considerable financial investment to see a medical discovery all the way to the point where it can help patients -- even with limited or no human testing. Due to financial or logistical reasons, many potential medical breakthroughs don't even make it through the experimental period, which may be why researchers dub it "the valley of death."
Pharmaceutical companies used to rely more on university research facilities or teaching hospitals -- which, in turn, gave them access to students who might appreciate a spring break full of experimental psychotropic drugs and repeat viewings of "The Wall." The downside to this, however, was that it introduced academic bureaucracy into an already highly regulated process. The FDA required the tests to be supervised by an institutional review board, and these were generally staffed by university faculty.
To streamline this ordeal, pharmaceutical companies now deal largely with commercial contract research organizations , which handle all the testing. In a 2008 article in The New Yorker, Carl Elliot described the resulting situation as a subculture of guinea pigs -- they even have their own publications, detailing which studies have the best pay and perks.
Cash Money for Human Guinea Pigs
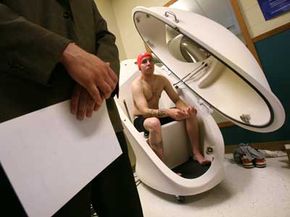
Paying human test subjects is a reality many view as unavoidable. While afflicted individuals might line up for the possible benefits of Phase III testing, Phase I testing tends to require healthy specimens. Like it or not, most of these individuals aren't going to volunteer without financial compensation.
This dilemma has existed for more than a century. In 1903, a New York physician stirred up ethical debate when he offered $5,000 to any man or woman willing to cut an ear off for his studies. Is it ethical to purchase a slice of another individual's health, even with the greater good in mind? Despite all the cozy accoutrements and oversight, paid test subjects put their health and even their lives on the line in sometimes painful or degrading clinical trials. After all, Phase I tests exist to help identify harmful side effects. If your bottle of medication says that it might result in bowel control problems or suicidal thoughts, you can bet that someone received a paycheck for experiencing them at some point.
Plus, there's the concern that the resulting guinea pig lifestyle winds up appealing to a particular segment of the general population. In some cases, the individuals are professional test subjects, moving from one to another like a jobless Phish fan trailing a never-ending tour. In other cases, the test ranks are occupied by some of the very underprivileged classes preyed upon in less ethical times:the poor, the mentally handicapped and even undocumented immigrants.
Contract research organizations have also come under fire for their oversight and staffing. University institutional review boards placed more emphasis on curtailing overzealous academics, in addition to testing ethics. For-profit review boards, however, answer to the market's need for speed, which has resulted in overlooked ethical concerns such as unsafe testing environments and unlicensed medical staff members. The FDA on the other hand largely places more emphasis on data inspections and reportedly inspects only 1 percent of clinical trials [source:Elliot].
Meanwhile, headlines continue to document the role of human embryonic stem cells in experimentation. While these highly versatile cells may play a huge role in the development of cures for various diseases and even ageing, many oppose the destruction of human embryos to get them.
In one form or another, human experimentation is as old as human curiosity. We learned that fire burned because we tested it. As scientific research continues, the challenge is to keep the flames in check.
Explore the links on the next page to learn even more about scientific experimentation.
Lots More Information
Related HowStuffWorks Articles
- How Biological and Chemical Warfare Works
- How Scientific Peer Review Works
- How the Scientific Method Works
- Are we on the brink of an AIDS vaccine?
- 10 Scariest Bioweapons
- How Stem Cells Work
More Great Links
- NOVA Online:The Holocaust on Trial
Sources
- "Ancient surgery:Alexandria." Channel 4. 2009. (March 17, 2009)http://www.channel4.com/history/microsites/H/history/a-b/ancientsurgery5.html
- Beagley, Sharon. "Where Are the Cures?" Newsweek. Nov. 10, 2008. (March 17, 2009)http://www.newsweek.com/id/166856
- Elliot, Carl. "Guinea-Pigging." The New Yorker. Jan. 1, 2008. (March 17, 2009)http://www.newyorker.com/reporting/2008/01/07/080107fa_fact_elliott
- Harris, Eleanor. "Eight scientists who became their own guinea pigs." New Scientist. March 11, 2009. (March 17, 2009)http://www.newscientist.com/article/dn16735-eight-scientists-who-became-their-own-guinea-pigs.html?DCMP=OTC-rss&nsref=online-news
- Longrigg, James. "Greek Rationale Medicine." Routledge. 1992.http://books.google.com/books?id=qD6G9R_-1UMC&pg=PA190&lpg=PA190&dq=vivisection+alexandria+account&source=bl&ots=Dfu9t_cG5A&sig=xUSLDKWh3NwCSyV-CfZoQUkDWOk&hl=en&ei=rn26SdW4OdTFtgeDk-ziDw&sa=X&oi=book_result&resnum=1&ct=result#PPP1,M1
- Lunenfeld, Bruno, et al. "Textbook of Men's Health and Ageing:2nd Edition." CRC Press. 2008http://books.google.com/books?id=9vEeMOwKY4AC&pg=PA5&lpg=PA5&dq=San+Quentin+Prison+took+part+in+testicular+transplant+experiments&source=bl&ots=EXzW5JjQk8&sig=VaiYKGZGUWKVGnClpMz2-UDOg9c&hl=en&ei=GGi-SbWKCMi0tweww-z3Cw&sa=X&oi=book_result&resnum=10&ct=result#PPR12,M1
- "Medical Ethics Timeline." ProQuest. 2009.
- "Results of Death-Camp Experiments:Should They Be Used?" NOVA Online. October 2000. (March 17, 2009)http://www.pbs.org/wgbh/nova/holocaust/experiments.html
- Roach, Mary. "Stiff:The Curious Lives of Human Cadavers." W.W. Norton &Company. 2003.
- Rodgers, Joann Ellison. "Guinea Pig Nation." Psychology Today. February 2009. (March 17, 2009)http://www.psychologytoday.com/articles/pto-20081215-000004.xml
- "Unit 731:Japan's biological force." BBC News. Feb. 1, 2002. (March 17, 2009)http://news.bbc.co.uk/2/hi/programmes/correspondent/1796044.stm
Sidste artikelSådan fungerer Mirages
Næste artikelSådan virker badesalt
 Varme artikler
Varme artikler
-
 Sådan konverteres europæiske højder til USAsMed undtagelse af Det Forenede Kongerige, hvor folk stadig bruger kejserlige enheder ved uformelle lejligheder, er måleenhedens forskel mellem USA (fødder) og Europa (meter). Dette udgør store problem
Sådan konverteres europæiske højder til USAsMed undtagelse af Det Forenede Kongerige, hvor folk stadig bruger kejserlige enheder ved uformelle lejligheder, er måleenhedens forskel mellem USA (fødder) og Europa (meter). Dette udgør store problem -
 Fleksibel fotonisk krystal fra flydende tynd-film metasurfaceSkematisk præsentation af TLD-filmdeformation, der danner optiske væskegitre (blå) på grund af overfladespændingseffekter udløst af interferens af overfladeoptiske tilstande (rød). (a) 2-D plasmonisk
Fleksibel fotonisk krystal fra flydende tynd-film metasurfaceSkematisk præsentation af TLD-filmdeformation, der danner optiske væskegitre (blå) på grund af overfladespændingseffekter udløst af interferens af overfladeoptiske tilstande (rød). (a) 2-D plasmonisk -
 Skilsmisse i en endimensionel verdenGrafik A viser atomkæden i kvantesimulatoren som enkeltbilleder af en video. Tiden løber fra top til bund. På toppen kan du se den uforstyrrede kæde. I den anden position sparkes et atom ud. Holon (ly
Skilsmisse i en endimensionel verdenGrafik A viser atomkæden i kvantesimulatoren som enkeltbilleder af en video. Tiden løber fra top til bund. På toppen kan du se den uforstyrrede kæde. I den anden position sparkes et atom ud. Holon (ly -
 At bremse spredningen af coronavirus i lukkede rum betyder bedre masker, tilstrækkelig ventilatio…Illustrationen viser rækkevidden af åndedrættet uden maske og under forskellige maske- og ansigtsskærmevalueringer. Kredit:Venugopal Arumuru/Indian Institute of Technology Bhubaneswar Med forskn
At bremse spredningen af coronavirus i lukkede rum betyder bedre masker, tilstrækkelig ventilatio…Illustrationen viser rækkevidden af åndedrættet uden maske og under forskellige maske- og ansigtsskærmevalueringer. Kredit:Venugopal Arumuru/Indian Institute of Technology Bhubaneswar Med forskn
- Copepoder:Havets ubesungne helte
- Hvordan er elementer dannet i stjerner?
- Krigshærdet Sydsudan er i alvorlig fare for klimaændringer
- Dine smartphone-apps sporer alle dine bevægelser:fire vigtige læsninger
- Vi har brug for en ny definition af pornografi – med samtykke i centrum
- Ulemper ved faktoranalyse